Endoscopic or Open Carpal Tunnel Release
Indications:
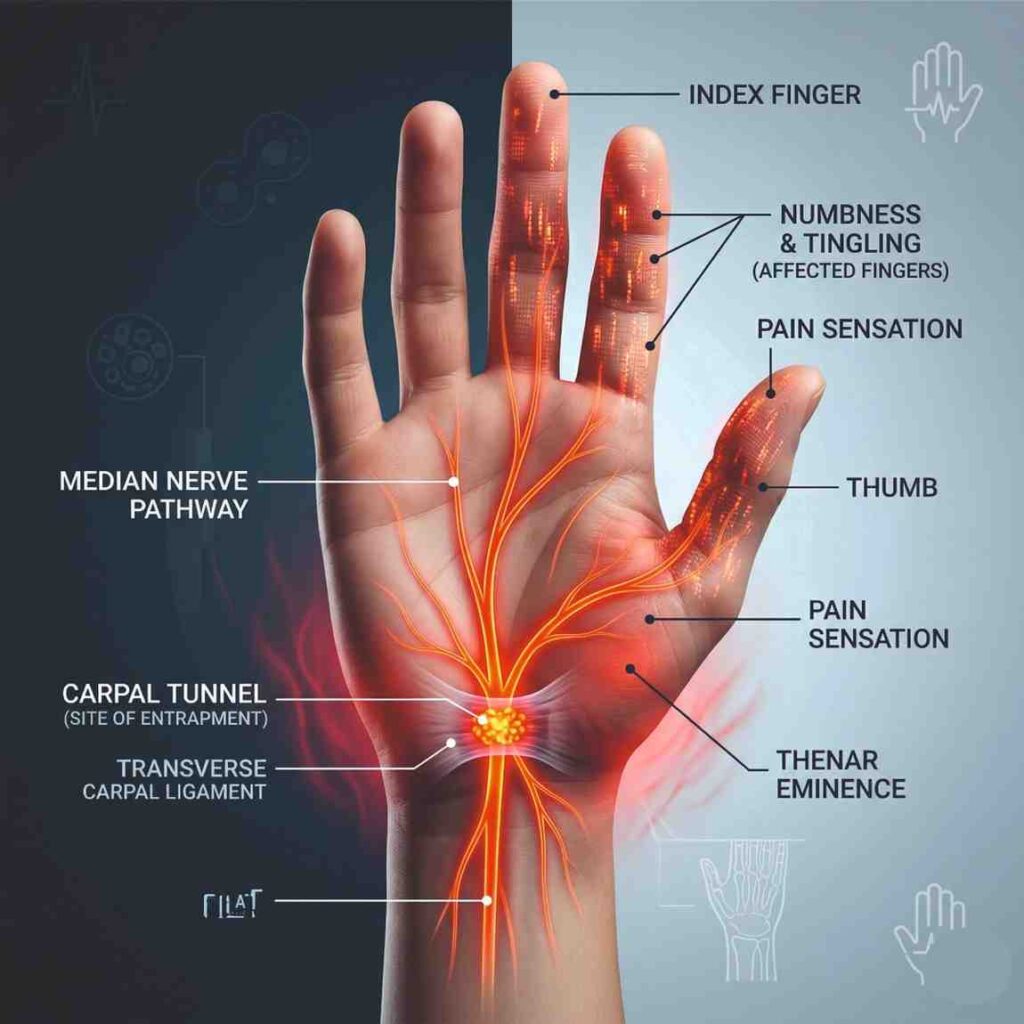
Carpal Tunnel Release surgery is recommended for patients with clinically significant carpal tunnel syndrome caused by compression of the median nerve at the wrist. Common symptoms include numbness, tingling, burning sensation in the thumb, index, and middle fingers, along with hand weakness and difficulty in gripping objects.
Diagnosis is usually confirmed with nerve conduction studies (NCS) or electromyography (EMG), which help assess the severity of nerve compression. Surgery is considered when conservative treatments such as wrist splinting, activity modification, medications, or local steroid injections fail to provide lasting relief. It is also advised in cases where there is progressive numbness, muscle weakness, or early signs of nerve damage.
Technique:
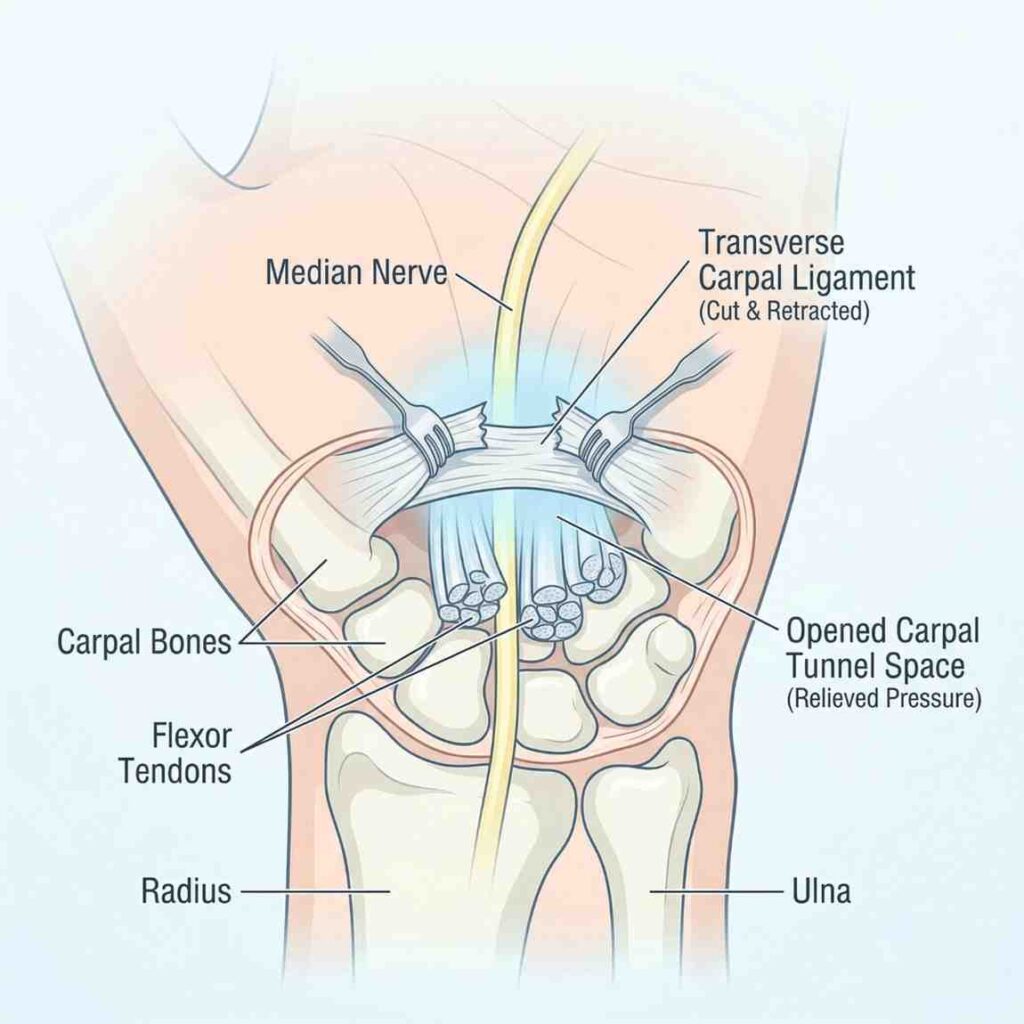
The procedure is performed under local or regional anesthesia in a sterile operating setting. The goal is to release the pressure on the median nerve by dividing the transverse carpal ligament (TCL), which forms the roof of the carpal tunnel.
Two commonly used surgical approaches are:
Endoscopic Technique:
A minimally invasive method where a small incision is made at the wrist crease. A thin endoscopic camera is inserted to visualize the undersurface of the ligament. The TCL is then carefully divided from inside, minimizing disruption to the overlying skin and soft tissues. This approach generally allows for quicker recovery and less post-operative discomfort.
Open Technique:
In this method, a small incision is made over the palm to directly expose the transverse carpal ligament. The ligament is then released under direct vision, ensuring complete decompression of the median nerve and its branches. This approach is particularly useful in complex or advanced cases.
Both techniques are safe and effective when performed with proper surgical precision.
Objective:
The primary objective of carpal tunnel release surgery is to achieve immediate decompression of the median nerve, thereby relieving pressure and preventing further nerve damage (axonal loss).
The procedure helps restore normal sensation, improve hand strength, and reduce symptoms such as numbness and tingling. Early intervention can significantly improve outcomes and allow patients to return to daily activities with better hand function and comfort.
1. When is carpal tunnel surgery needed?
Surgery is recommended when symptoms like numbness, tingling, or hand weakness do not improve with splints, medications, or injections. It is especially important if nerve tests show significant compression.
2. What is the difference between endoscopic and open surgery?
Endoscopic surgery uses a small camera and smaller incision, leading to quicker recovery. Open surgery involves a slightly larger incision but allows direct visualization, which can be useful in complex cases.
3. Is carpal tunnel surgery painful?
The procedure itself is done under anesthesia, so there is no pain during surgery. Mild discomfort after surgery is common but manageable with medication.
4. How long does it take to recover after surgery?
Most patients notice symptom relief within a few days to weeks. Full recovery and return to normal hand strength may take a few weeks depending on the severity.
5. Will numbness go away completely after surgery?
In many cases, numbness improves significantly. However, if the nerve was compressed for a long time, recovery may take longer or may not be complete.
6. When can I use my hand normally again?
Light activities can usually be started within a few days, while full use of the hand may take a few weeks after proper healing.